Gladstone NOW: The Campaign Join Us on the Journey✕

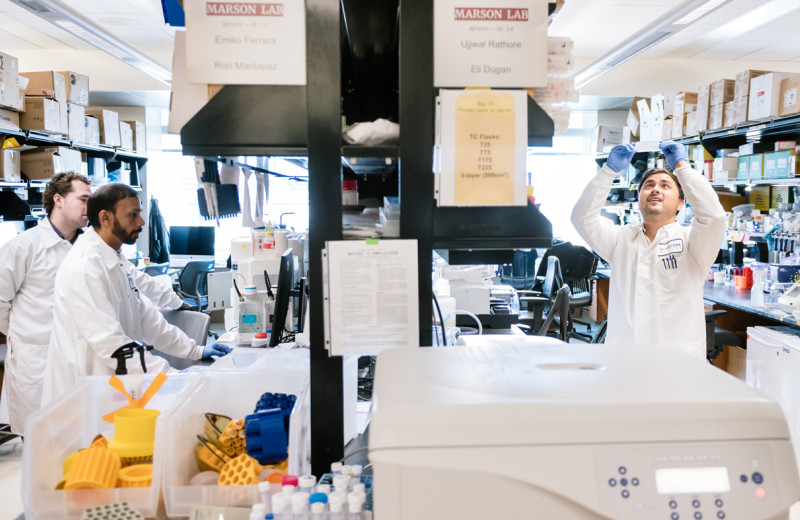
Gladstone scientists are studying hantaviruses and other viruses with pandemic potential, with the goal of developing broad-acting antiviral therapies.
The international health community is on high alert, tracing a silent, high-stakes trail left by the MV Hondius cruise ship.
What began as a birdwatching excursion in Argentina has transformed into a multi-national health crisis. With three confirmed deaths, several passengers in intensive care units across Europe and South Africa, a person in Switzerland testing positive, and more than 30 passengers—including several in the US—under surveillance, the primary concern is no longer just the virus itself. The concern is how it’s spreading.
While most hantaviruses are contracted through inhalation of rodent droppings, health authorities have confirmed this outbreak involves the Andes strain, the only variation known to spread from person to person.
As the World Health Organization intensifies its monitoring, we spoke with virologist Melanie Ott, MD, PhD, director of the Gladstone Infectious Disease Institute, where she and other scientists are studying hantaviruses. She sheds light on the science behind the headlines and why this specific event has public health experts on edge.
Ott and her lab are working on hantaviruses because there are currently no vaccines or treatments—their goal is to find broad and rapidly deployable antivirals.
We’re hearing that dozens of cruise ship passengers who may have been exposed to the virus left the ship before the full scale of the outbreak was known. Why is this causing so much concern?
The concern stems from the specific strain involved. Most hantaviruses have very low person-to-person transmissibility; you usually need to be in close contact with rodent feces to get infected and sick. But the Andes strain, which is endemic to Argentina, has a documented ability to spread between humans. For this to happen, you usually have to be in close contact with an infected person.
When you have an outbreak in a closed environment like a cruise ship or an airplane, that risk escalates. We’re seeing a timeline where people became sick, the virus spread on the boat, and now we have cases involving people who flew home before knowing that they were exposed or when they were already sick. That led to a flight attendant being hospitalized due to a possible infection. All of this indicates a chain of transmission that bypasses rodents.
The incubation period for this virus is unusually long. How does that complicate efforts to contain it?
It’s a major challenge. The incubation time—after infection, but before symptoms are apparent—is highly variable. While usually occurring between two and three weeks, it can be anywhere from 10 days up to eight weeks. This makes it incredibly hard to trace exactly when and where a person was infected and who they were in contact with. Because some passengers disembarked and scattered to different countries before they became sick, health officials are essentially chasing the virus across the globe.
For those who do get sick, what does the clinical progression look like? We’ve heard the term “rapid decline” used frequently.
It’s a tragic clinical picture. It starts with very non-specific, flu-like symptoms—fever, muscle aches, cough. But then, very suddenly, the patient can take a dramatic turn for the worse.
With the Andes strain, you often see a massive inflammatory reaction that leads to edema (swelling) and cardiopulmonary failure. It has a mortality rate of roughly 40 percent or higher. If you’re in a remote area or on a ship without access to advanced life support and mechanical ventilation, it can be very difficult to survive.
Can doctors use a vaccine or treatment for those who’ve been exposed to the virus or contracted it?
Currently, no. There are no approved vaccines and no specific antivirals known to be effective against hantavirus. Treatment is almost entirely supportive—keeping the lungs and heart functioning while the body fights the virus.
At Gladstone, we’re working on a different approach. Similar to what we did with COVID-19, together with the lab of Nevan Krogan, PhD, we’re looking for “druggable” factors in the body. Instead of trying to attack the virus directly, we track proteins in human cells that the virus needs to replicate. If we can block those, we can stop the virus from proliferating.
You often talk about the need for better pandemic preparedness. In an ideal world, how would authorities be able to respond to an outbreak situation such as this one?
Ideally, we should have medicines known as “neutralizing antibodies” stored and ready for deployment. These are specialized immune proteins that attach to the surface of viruses and prevent entry into the cell, thereby stopping infection. If health agencies had a stockpile specific to the Andes strain, they could have boarded that cruise ship and given everyone on board an antibody shot to protect them immediately. This is often referred to as “passive immunization.”
“I don’t believe this is a highly transmissible virus in the way COVID-19 was. However, we cannot ignore it. Hantavirus cases are increasing, the hits are coming closer, and the WHO’s involvement tells us this is a serious threat.”
The problem is that this approach isn’t seen as commercially viable because these outbreaks are sporadic. But this is exactly what pandemic preparedness looks like: investing as a society in effective tools for the potential future event so we aren’t caught off guard when a ship like this arrives in port.
We are working on hantaviruses at Gladstone precisely because there are currently no vaccines or treatments; our primary goal is to find antivirals that are broad and rapidly deployable, and we have some promising leads. We have world-class mRNA vaccine expertise in the lab of Magnus Hoffmann, PhD, to support new vaccine development.
Coincidentally, the Gladstone Infectious Disease Institute just hosted a visiting scientist from Chile who’s an expert in Andes virus and with whom we’re currently in close contact.
Finally, should the general public be worried about this becoming a new global pandemic?
I don’t want to create panic. And I don’t believe this is a highly transmissible virus in the way COVID-19 is. It seems to require these “incubating environments”—close-contact, closed-loop settings—to spread effectively between people.
However, we cannot ignore it. Hantavirus cases are increasing, the hits are coming closer, and the WHO’s involvement tells us this is a serious threat. We need to learn our lessons now and invest in diagnostics, vaccines, and treatments before the next dangerous virus rears its head.
Melanie Ott, MD, PhD, is a virology expert and director of the Gladstone Infectious Disease Institute. Ott serves as Gladstone’s Nick and Sue Hellmann Distinguished Professor and director of the Michael Hulton Center.
Scientists Map How HIV Hijacks Human Cells—and How Cells Can Fight Back
Scientists Map How HIV Hijacks Human Cells—and How Cells Can Fight Back
A new genetic roadmap reveals hundreds of hidden players in HIV infection, including two proteins that stop HIV in its tracks.
News Release Research (Publication) HIV/AIDS Genomic Immunology Krogan Lab Marson LabCould This Molecule Be ‘Checkmate’ for Coronaviruses?
Could This Molecule Be ‘Checkmate’ for Coronaviruses?
Scientists develop powerful drug candidates that could head off future coronavirus pandemics.
News Release Research (Publication) COVID-19 Infectious Disease Krogan Lab Ott LabUnderstanding How the Immune System Switches Between Rest and Action
Understanding How the Immune System Switches Between Rest and Action
Scientists at Gladstone and UCSF discover how one protein controls the behavior of immune cells, with potential applications for treating cancer and autoimmune conditions.
News Release Research (Publication) Autoimmune Diseases Cancer Genomic Immunology Krogan Lab Marson Lab CRISPR/Gene Editing