Gladstone NOW: The Campaign Join Us on the Journey✕

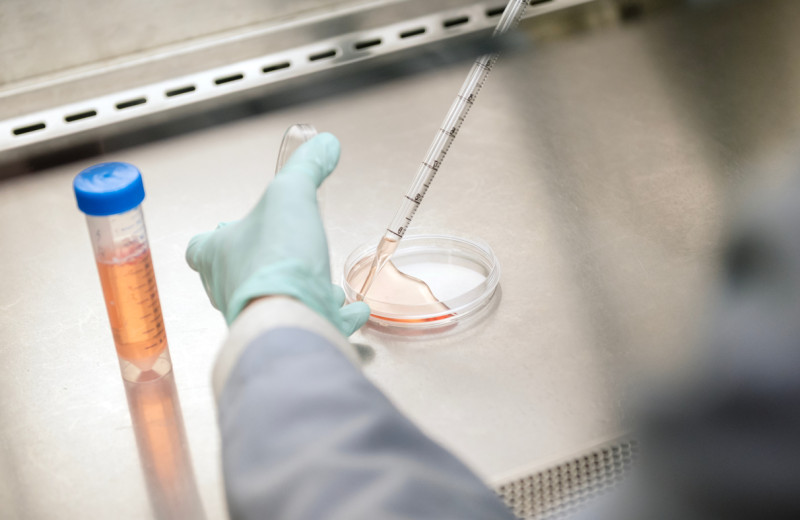
A fast and powerful new gene-editing technology called CRISPR is changing biomedical research, and it has the potential to do much more. Gladstone President R. Sanders "Sandy" Williams, writes about several key questions that need to be answered before scientists start using this method to rewrite genomes outside of the laboratory. [Photo: Chris Goodfellow]
We’ve all heard about reading the human genome—deciphering the alphabet of As, Cs, Ts, and Gs that make up our genes and determine who we are. But did you know that we now can write our DNA as well?
A powerful, new biological tool called CRISPR (clustered regularly interspaced short palindromic repeats) allows us to edit a cell’s DNA, inserting or deleting a string of code, or even swapping one letter for another with unprecedented speed and precision. This remarkable technology can rewrite gene sequences, or turn genes on and off, and it has the potential to change entire species of plants and animals.
However, with great power should come great responsibility, and as a society we must decide how this technology should be applied in a responsible manner.
Where Did CRISPR Come From?
Like many scientific advances, CRISPR came about through research into a seemingly unrelated biological question. Jennifer Doudna, PhD, a molecular biologist at UC Berkeley, is credited with developing CRISPR. However, Dr. Doudna did not set out to invent a new technology to change our genes, she wanted to learn how single-celled organisms like bacteria fight off viruses.
With considerable ingenuity, Dr. Doudna recognized that a system bacteria use to inactivate viral invaders could also be employed to edit the genome of any cell, human or otherwise. Thus, a seemingly esoteric basic science discovery has led to a remarkable scientific advance with impact across all of biology.
Although CRISPR is not the first gene-editing technology, it has properties that exponentially exceed those of previous methods. For several decades, scientists have had the ability to edit a cell’s DNA, but in comparison to CRISPR, the methods have been expensive, inaccurate, inefficient, and capable of inflicting significant collateral damage to the genome. CRISPR, on the other hand, is efficient and precise, able to pinpoint a single location within chromosomes. If the old methods are analogous to dropping megaton bombs on the genome, CRISPR is more akin to a smart drone directing a payload precisely to a small target
How Does CRISPR Work?
First, CRISPR works as a guide, allowing scientists to focus on the precise stretch of DNA they want to edit. We humans have a staggering three billion letters in our genome. CRISPR uses little snippets of RNA ten to twenty letters long to locate an identical letter string in a cell’s DNA. Even within our enormous genome, it is possible to design an RNA string that corresponds to one and only one place within our DNA. In other words, CRISPR allows scientists to find, and act upon, a single piece of straw in a three billion piece haystack.
The second key component to CRISPR is a protein called Cas9 (or a modified variant thereof) that is attached to the RNA string and can cut the DNA at the targeted location. This molecular scalpel enables scientists to perform surgery on the genome, swapping, adding, or deleting letters. And by changing the letters, the scientists can change the gene, which in turn alters the cell’s behavior and fate.
What Are the Applications?
An immediate use of this technology in the laboratory is to advance our understanding of how the human body works and how genetic mutations lead to disease. For example, my colleagues at the Gladstone Institutes are using CRISPR to investigate and correct gene mutations that cause cardiovascular disease, and to develop technologies for heart regeneration. They do this in the lab in heart cells derived from induced pluripotent stem cells (iPSC)—stem cells that have been created from a patient’s skin cells that can turn into brain, heart, liver, and insulin-producing pancreas cells. This combination of two revolutionary research tools—iPSC and CRISPR—will accelerate the development of new treatments for vicious unsolved diseases such as heart failure, Alzheimer’s disease, diabetes, and deadly viruses.
Going a step further, CRISPR can be used to rewrite the genome of plants, animals, and human beings. For instance, it is technically feasible even today to take stem cells from a patient’s bone marrow, edit the cells’ DNA, and insert them back into the patient, where the revised cells would proliferate throughout the body.
In principle, such a method could be useful to correct inherited blood disorders such as sickle cell anemia, or to make individuals resistant to viruses like HIV. Scientists already know about a protein on the surface of our white blood cells that, if removed, prevents HIV from infecting the cell. Persons naturally lacking this protein appear to be healthy, indicating that removing it should be safe.
CRISPR can also edit genes in human embryos. Some scientists in China have already done this, though they did not achieve their technical aims and did not allow the embryos to develop beyond an early stage. Nevertheless, in skilled and responsible hands, and with appropriate safeguards, this technology presents opportunities to repair gene mutations that otherwise after birth would cause devastating diseases like Huntington’s disease. It is most important to understand, however, that any DNA that is rewritten in human embryos will be passed on to future generations—all of the offspring will inherit the edits, and those changes will be in the human germline of any descendants forever. This is not the case with applications where gene editing would affect only the individual.
What Are The Tough Questions?
I’ve mentioned several potentially valuable uses of CRISPR, but it is easy to imagine applications that are disturbing. Inexpert or irresponsible use of CRISPR to alter genomes of human embryos could result in great harm. As a society, we need to decide how this technology should be regulated.
First and foremost, I favor a moratorium on gene editing to alter the human germline until the technology is fully understood and perfected, and until a broad consensus on guidelines for responsible use can be achieved. We cannot be confident yet that we know how to avoid unexpectedly deleterious consequences, and we do not yet have a clear line of demarcation separating beneficial applications (e.g. correcting an inborn error that would result in a damaged child) from those of dubious social value (e.g. designer babies engineered to be taller, smarter, or more beautiful).
Determining the circumstances in which the technology can and should be applied brings a cascade of questions: When is a gene editing technology safe and effective enough to be used outside of the laboratory? How do we balance risks and benefits appropriately? How far should we go in altering the future genetic landscape of free-living species, including humans? And importantly, who should decide such issues?
CRISPR-based research tools already are accelerating the pace at which we can understand fundamental mechanisms of how things work in our cells and our bodies, and what goes wrong when we become ill or impaired. Work of this nature merits aggressive support without hesitation. As for using CRISPR to rewrite the genomes of human embryos, or of plants and animals in the wild, a slower and more measured pace is warranted.
Reading and writing the human genome is real, here and now. What comes of this is a matter for all of us, and not scientists alone, to guide.
R. Sanders Williams, MD, is President of the Gladstone Institutes and Gladstone's Robert W. and Linda L. Mahley Distinguished Professor. He is also a Professor of Medicine at the University of California, San Francisco (UCSF).
For more stories about Gladstone's cutting-edge biomedical research, visit our News & Highlights.
Want to Join the Team?
Our people are our most important asset. We offer a wide array of career opportunities both in our administrative offices and in our labs.
Explore CareersA Universal Toolkit for Editing Bacterial DNA
A Universal Toolkit for Editing Bacterial DNA
Scientists at Gladstone expanded their retron-based genome editing technology beyond E. coli, showing it works in 15 diverse bacterial species.
News Release Research (Publication) Data Science and Biotechnology Shipman Lab CRISPR/Gene EditingGladstone Expands Research Footprint With 105,000 Square Feet of New Laboratory Space
Gladstone Expands Research Footprint With 105,000 Square Feet of New Laboratory Space
Gladstone Institutes is adding state-of-the-art laboratories in a newly constructed Mission Bay building.
History Institutional News News Release Genomic Immunology Data Science and Biotechnology Marson Lab Pollard Lab AI CRISPR/Gene Editing GenomicsGene Editing Strategy Could Treat Hundreds of Inherited Diseases More Effectively
Gene Editing Strategy Could Treat Hundreds of Inherited Diseases More Effectively
Scientists at Gladstone show the new method could treat the majority of patients with Charcot-Marie-Tooth disease.
News Release Research (Publication) Neurological Disease Conklin Lab CRISPR/Gene Editing